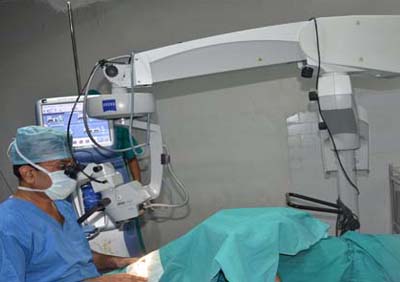
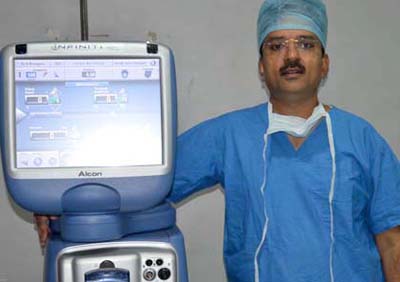
The Normal Cornea
The eye is like a camera in which lenses focus the picture on a light sensitive film. In the human eye, the transparent cornea and lens focus light on the retina, which changes it into electrical signals, which are then transmitted to the brain by the optic nerve to be perceived as images.
The cornea is the front transparent window of the eye and forms the outermost one-sixth of the eyeball. It is lamellar in nature (like plywood) and is made up of 5 layers, each of which has a definite function. In order to be effective it must remain transparent. Freezing, heating, molding, lathing, tattooing, excising, incising and transplanting are all means by which the delicate and sensitive cornea has been altered for optical, therapeutic and cosmetic purposes. Due to absence of blood vessels in the cornea, much of its oxygen requirement comes from atmospheric oxygen dissolved in the tear film. When the eyelids are closed, oxygen enters the cornea from the superficial conjunctival vessels. Nutrients needed for the cornea pass into it by diffusion. Hence, carbon dioxide and waste products are also removed across the tear film. Hence, any deficiency of the tear film will directly or indirectly affect the cornea.
What is Keratoconus?
Normally the cornea is nearly spherically shaped thus allowing light to be focused clearly on the back of the eye (retina). However in a condition called Keratoconus, the cornea begins to thin, and this allows the normal pressure of the eye to make the cornea bulge forward taking on a cone-shape. As the cornea gradually becomes more cone-shaped, the vision blurs and becomes distorted due to a high degree of astigmatism. Initially vision may be correctable with spectacles, but as the condition progresses, and the cornea becomes more irregular causing distorted vision, spectacles become less effective. In such a situation, contact lenses not only provide better vision, but also help to retard the progress of the disorder. A rigid contact lens (RGP / "semi-soft" contact lenses) must be used, so that it can hold its shape, as a soft lens would simply mould to the existing shape and thus not allow complete correction of the problem. Sometimes the patient is fitted with soft lenses (for comfort), over which semi-soft lenses are fitted ("piggy-back" lenses).
Fitting contact lenses for keratoconus requires expertise. Well-fitting contact lenses dramatically improves such a patient's vision to nearly that of a normal person's, and significantly improves his or her quality of life. Any excessive pressure of a poorly fitting lens on the cone apex can cause permanent scarring within months or years (This scarring can also occur naturally). For this reason it is important for regular follow-up visits to be made so that any corneal changes that have occurred can be compensated for in the design of a new lens. It is quite common for patients to be refitted at irregular intervals as the condition progresses. Rarely, scarring is so severe that a corneal graft (transplant) is necessary.
A recent promising treatment modality for keratoconus is C3R (Corneal Collagen Cross-linking).
What is Corneal Collagen Cross-linking (C3R)?
Cross Linking of Cornea Collagen (C3R) is a process to increase the mechanical stability of corneal tissue. The aim of this treatment is to create additional chemical bonds inside the corneal stroma by means of a highly localized photo polymerization.
The indications for cross linking today are corneal ectasia the disorders such as keratoconus and pellucid marginal degeneration, iatrogenic keratectasia after refractive lamellar surgery and corneal melting that is not responding to conventional therapy.
The History of Corneal Cross-linking
The procedure was developed from 1993 till 1997 by Prof. Theo seiler and Prof. Eberhard Spoeri at the University of Dresden, Germany. The first patients were treated in 1998. Today corneal cross-linking is performed in more than 300 centers around the world. Corneal Cross-linking has the potential to become the standard treatment for keratoconus thus preventing the need for penetrating keratoplasty!
The Principle of C3R
Photo-polymerization using UV-light was found to be the most promising technique to achieve cross-links in connective tissue. Photo-polymerization is activated by means of a non-toxic and soluble photomediator and a wavelength which is absorbed strongly enough to protect deeper layers of the eye (riboflavin-UVA technique).
UV-A radiation with concomitant administration of riboflavin solution leads to physical cross linking of the corneal collagen fibers.
Thus progressive corneal thinning is slowed down or even stopped and the Bio-mechanical strength of corneal tissue is improved.
The Device for C3R
For C3R we need riboflavin dye and a special device called cross-linker. Cross linker is a device to deliver UV-A light of specific wavelength of 365 nm , at controlled energy level of 3 mW/cm.sq.
The C3R Procedure
After removal of the corneal epithelium, riboflavin solution is instilled for 30 minutes on to the cornea. Then the corneal penetration of this is checked by establishing that the anterior chamber is slightly yellow. Pachymetry is performed to make sure that minimum corneal thickness is maintained.
UV-A radiation starts under continued administration of Riboflavin Solution. After 30 minutes of radiation treatment is finished and the patient receives post-operative treatment like after a PRK procedure. A bandage contact lens is inserted in the operated eye and the patient is administered oral and topical antibiotics, steroids, anti-inflammatory medication as well as lubricant eye drops.
Clinical Experience with C3R
Today, more than 1,400 eyes have been cross-linked world wide in controlled clinical studies with a follow up to 5 years.
Clinical studies have shown a significant increase in best corrected visual acuity (BCVA) in more than 85% of the treated eyes.
Six months after corneal cross-linking the refractive cylinder was reduced in over 80% of the eyes.
The steepest K-value was usually decreased by 1 diopter and the percentage of eyes that had a clinical relevant reduction exceeds 86%.
Safety of C3R
Corneal cross-linking is considered to be a safe procedure, provided the recommended safeguards are observed. Up until today no sight threatening side effects have been reported.
An excellent Vision Correction Option
The ICL (Implantable Contact Lens) is a state-of-the-art refractive error solution that is ideal for anyone who has the need or desire for removal of power with high quality of vision correction. ICL or Implantable Contact Lens, as the name suggests, is a kind of lens which is implanted into the eye and does not require frequent removal like a normal contact lens. This phakic intraocular lens has numerous advantages including its correction of the widest range of myopia (near sightedness), hyperopia (far sightedness) and astigmatism (cylindrical power).
* ICL can correct a wide range of vision errors by permanently inserting a Contact lens in front of the natural lens of the eye.
- ICL is a kind of soft contact lens which is inserted into the eye through a very small incision
- Just like LASIK or Wavefront Lasik it takes only 5-10 minutes for the procedure
- The lens is customized according to each eye's shape and size
- Widest power correction range from +10D to -20D with cylinder upto 6D
- Made from a material called "Collamer" which is bio compatible (safe to stay in the eye for very long time)
- This new technique is similar to cataract surgery, but the natural lens remains in place so the eye's natural focusing ability is preserved.
- An implantable contact lens is beneficial because it becomes a permanent fixture of the eye, avoiding time consuming maintenance.
- It does not get lost, or have to be replaced like glasses and contact lenses.
- ICL procedures are being used on highly nearsighted and farsighted patients who may not be candidates for the more common laser procedures such as LASIK, LASEK, and PRK. Unlike laser vision correction procedures that permanently change your vision, it is possible to later remove an ICL.
How do I know if I am a suitable ICL candidate?
- Candidates for the ICL are above 18 years of age, suffer from myopia (nearsightedness),hyperopia (farsightedness) and/or astigmatism (cylindrical power) and want to experience superior vision correction.
- Candidate with refractive error who are unsuitable for laser refractive surgery.
- Prospective person should consult his/her ophthalmologist (eye surgeon) for more information, including an assessment of their candidacy.
- Women who are pregnant or nursing should wait to have the ICL implanted. Lastly, those without a large enough anterior chamber depth or endothelial cell density may not be a good ICL candidate.
Advantages of ICL?
- No blood! No pain! No hospitalisation!
- Almost all levels of power can be treated
- Excellent quality of vision
- Easily removed or replaced (5-10 minutes)
- Cosmetically good as it's INVISIBLE!!
- Fast recovery
Why Patients Seek ICL
Patients seek the ICL because they expect the highest quality of results from their refractive vision correction procedure. The advantages of this phakic IOL (highlighted below) make the ICL a sought after treatment for nearsightedness & farsightedness.
High quality of vision The ICL not only corrects your refractive power or number, but it also enhances your quality of vision by producing sharp vision.
Wide treatment range In comparison to other refractive procedures, the ICL offers the widest treatment range for correction of vision.
Foldable because the ICL is foldable, a small incision is required during the procedure. This feature makes the procedure efficient (no sutures needed) and improves healing time.
Invisible the placement of the ICL into the posterior chamber of the eye makes the lens invisible to both the patient and any observer.
Collamer composition Collamer is made from collagen, which is a substance that naturally occurs in the body. This makes the lens highly biocompatible with the eye.
Proven track record Implanted in over 65,000 eyes worldwide, the safety and amazing improvement in vision quality of the ICL has been proven over the last 15 years.
Because the ICL is also ideal for patients with contraindications for laser refractive surgery, some people may consider the ICL as an alternative to LASIK; however, as you can see, it is so much more than that. It is often compared to the corneal refractive procedure because the ICL takes refractive surgery beyond the limits of LASIK. Patients, who may not discover the ICL until they begin to search for an alternative treatment to avoid LASIK or PRK, realize that the ICL is not just an alternative; it is the good choice for superior vision quality.
Advantages of ICL
- Preserves accommodation
- No corneal tissue removed
- Retains corneal asphericity
- Possibly retains contrast sensitivity
- Removable
How does the ICL work?
- Similar to a contact lens
- Designed to remain inside the eye
- Doesn't get dirty and needs no maintenance unlike a contact lens
- Once-a-year visit to hospital recommended for examination
How does the ICL differ from other refractive procedures?
- Does not cut or remove tissue from the cornea
- Cornea retains it natural shape
- Safer for higher degrees of myopia, hyperopia, astigmatism and thin corneas
- Less glare issues on patients with large pupils
- Very stable over time, no regression
What to expect on the procedure?
- Procedure should take 10-15 minutes per eye
- Laser Iridotomies done prior to surgery
- Dilating and anesthetic drops
The ICL Procedure:
- The implant surgery is quick and painless, lasting only about 10 – 15 minutes.
- The area around your eyes will be cleaned and a sterile drape may be applied around your eye.
- Eye drops or a local anesthetic will be used to numb your eyes.
- When your eye is completely numb, an eyelid speculum will be placed between our eyelids to keep you from blinking during the procedure.
- The recovery time is short and the results of the surgery are almost immediate.
- Most patients resume normal activities within a week.
Potential ICL risks include:
- Overcorrection: This complication occurs if the prescriptive power of the implanted ICL is too strong. In most cases it can be corrected with corrective eyewear or with an ICL replacement.
- Undercorrection : The opposite of overcorrection, undercorrection is the result of an implantable contact lens with too weak of a prescription.
Correction methods are similar to those of overcorrection.
- Infection During most surgeries, there is a potential of an infection.
- Increased intraocular pressure Pressure may build in the eye after an ICL procedure. The sooner a surgeon is alerted to this, the greater the chance of avoiding serious damage.
- This is detected during your follow up visits with us or in case you face acute blurring of vision or headaches, you must visit the eye clinic
- ICLs have the potential, however slight, of needing to be repositioned.
- Damage to crystalline lens : because implantable contact lenses are implanted into the eye, there is a potential that the eye's natural lens may be damaged during the procedure. If the damage is severe, the crystalline lens may need to be replaced with an intraocular lens.
- Cataract development : Over 50 percent of the population will develop cataracts by the age of 65, however, it is believed that the use of some implantable contact lenses may cause cataracts at an earlier age, this however is rare.
- Halos, glare, and double vision : Updated ICL models greatly diminish the risks of halos, glare, and double vision.
- Retinal detachment : Less than 1 percent of patients in the clinical studies were affected by retinal detachment. It should be noted, however, that the occurrence of retinal detachment increased as the degree of myopia increased.
Where is the ICL placed?
A trained ophthalmologist will insert the ICL through a small micro-incison, placing it inside the eye just behind the iris in front of the eye's natural lens. The ICL is designed not to touch any internal eye structures and stay in place with no special care.
What is Toric ICL?
The Toric ICL is only a variant of ICL. Toric ICL corrects your nearsightedness as well as your astigmatism (cylindrical power) in one single procedure. Each lens is custom made to meet the needs of each individual eye.
What is the track record of the ICL?
Prior to being placed on the market, the ICL was subject to extensive research and development. Today,more than 65,000 patients worldwide enjoy the benefits of the device. In an USFDA clinical trial, over 99 percent of patients were satisfied with their implant. The ICL has a track record of stable, consistently excellent clinical outcomes. The lens has been available internationally for over 12 years.
Does it hurt?
No, most patients state that they are very comfortable throughout the procedure. Your ophthalmologist will use a topical anesthetic drop prior to the procedure and may choose to administer a light sedative as well.
What is the ICL made of?
The ICL is made of Collamer®, a highly biocompatible advanced lens material which contains a small amount of purified collagen. Collamer does not cause a reaction inside the eye and it contains an ultraviolet filter that provides protection to the eye. Collamer is a material proprietary to STAAR Surgical Company, the company that manufactures ICL.
What if my vision changes after I receive the ICL?
One advantage of the ICL is that it offers treatment flexibility. If your vision changes dramatically after receiving the implant, your doctor can remove and replace it. Patients can wear glasses or contact lenses as needed following treatment with the ICL. The implant does not treat presbyopia (difficulty with reading in people 40 and older), but you can use reading glasses as needed after receiving the ICL.
What type of procedure is involved in implanting the ICL?
The implantation procedure for the ICL (Implantable Contact Lens) is refractive eye surgery that involves a procedure similar to the intraocular lens (IOL) implantation performed during cataract surgery. The main difference is that, unlike cataract surgery, the ICL eye surgery does not require the removal of the eye's natural lens. The ICL procedure is a relatively short outpatient procedure that involves several important steps. The surgical procedure to implant the ICL is simple and nearly painless.
As a ICL candidate, your doctor will prepare your eyes one to two weeks prior to surgery by using a laser to create a small opening between the lens and the front chamber of your eye (iridotomy). This allows fluid to pass between the two areas, thereby avoiding the buildup of intraocular pressure following the surgery. However, some surgeons choose to do this step on the same day of the surgery. The implantation procedure itself takes about 10-15 minutes and is performed on an outpatient basis, though you will have to make arrangements for someone to drive you to and from the procedure.
You can expect to experience very little discomfort during the ICL implantation. You will undergo treatment while under a light topical or local anesthetics. Following surgery, you may use prescription eye drops or oral medication. The day after surgery, you will return to your doctor for a follow-up visit. You will also have follow-up visits one month and six months following the procedure.
Although the ICL requires no special maintenance, you are encouraged to visit your eye doctor annually for check-ups following the ICL procedure.
Can the ICL be removed from my eye?
Although the ICL is intended to remain in place permanently, a certified ophthalmologist can remove the implant in a very quick & short procedure.
Is the ICL visible to others?
No, the ICL is positioned behind the iris (the colored part of the eye), where it is invisible to both you and observers. Only your doctor will be able to tell that vision correction has taken place.
Will I be able to feel the ICL once it is in place?
The ICL is designed to be completely unobtrusive after it is put in place. It stays in position by itself and does not interact with any of the eye's structures.
Where can I get my ICL procedure done?
Please be aware that ICL procedure is presently available at select centre`s & hospitals in India as it requires precision and skills. In our Institution our Cornea and LASIK experts will guide you better if you are the right candidate for this procedure.